A group of independent vaccine advisers to the US Centers for Disease Control and Prevention is meeting this week, with a primary focus on the hepatitis B vaccine, reports BritPanorama.
Following presentations on hepatitis B and the vaccine’s safety, the Advisory Committee on Immunization Practices (ACIP) is set to vote on whether to discontinue the universal recommendation for the hepatitis B vaccine for infants.
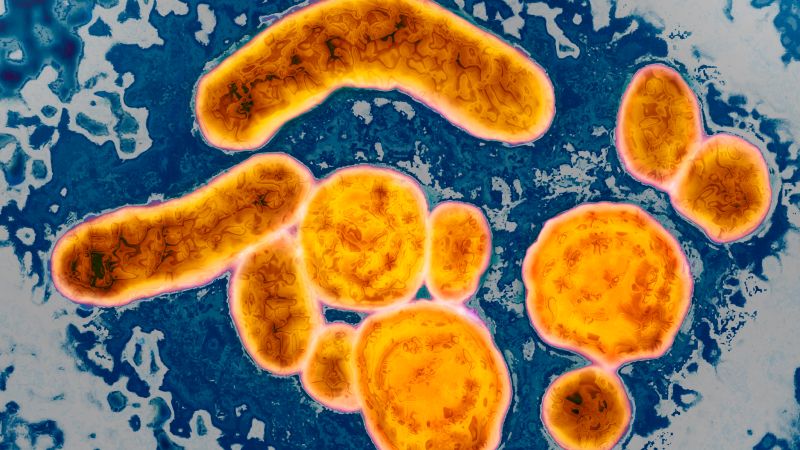
What is hepatitis B?
Hepatitis B is a liver infection caused by a virus. After an acute hepatitis B infection, many adults clear the virus; however, acute infections can develop into chronic hepatitis B, which is linked to severe health risks, including liver cancer, organ failure, and cirrhosis. Individuals with chronic hepatitis B may experience a 70 to 85% increased risk of early death.
During Thursday’s ACIP meeting, Dr. Sandra Fryhofer, a liaison for the American Medical Association, shared her experiences treating hepatitis B patients as a medical student. “Those were the sickest patients I had ever seen in my life,” she stated. “I have treated patients that have liver disease from hep B, cirrhosis from hep B, liver cancer from hep B, and death from hep B.”
Infants and children infected with hepatitis B are more likely to develop chronic conditions, with approximately 90% of infants and 30% of children aged 1 to 5 at risk of progressing to chronic disease.
How is hepatitis B spread?
The hepatitis B virus is highly infectious, transmitted through contaminated blood, semen, or other bodily fluids from an infected individual. Certain behaviors, such as intravenous drug use and sexual activity, can elevate the risk of transmission. Moreover, the virus can be passed from an infected mother to her child during childbirth.
How common is hepatitis B?
A significant number of individuals with hepatitis B remain asymptomatic, with over half unaware of their infection. The latest data from the CDC indicates around 2,200 newly reported acute hepatitis B cases in 2023, but estimates suggest that the actual number could exceed 14,400. The CDC also estimates that about 640,000 adults in the US live with chronic hepatitis B. Globally, the World Health Organization estimates that approximately 254 million people have chronic hepatitis B, with around 1.2 million new infections occurring each year.
Can hepatitis B be treated?
Currently, there is no treatment for acute hepatitis B, though medications are available for chronic cases, which may require lifelong management.
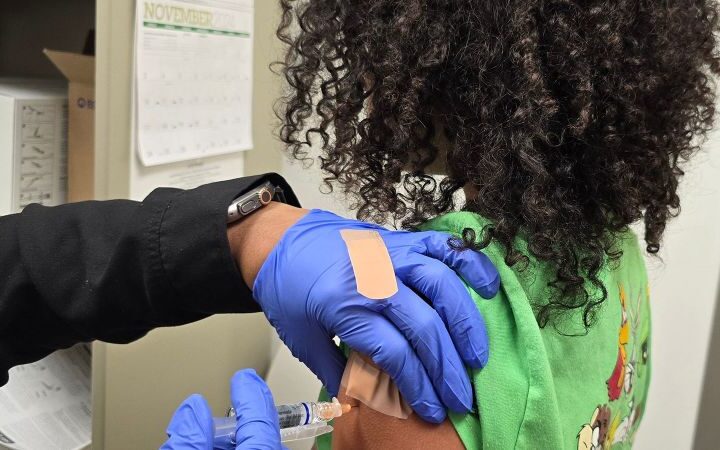
How can hepatitis B be prevented?
The most effective way to prevent hepatitis B infection is through vaccination. The vaccine shows high efficacy in infants and provides lasting protection into adulthood. The CDC recommends that all infants receive the hepatitis B vaccine at birth, while ensuring that a scientific review shows 95% of healthy infants develop strong protection against infection after a three-dose series. Vaccination is shown to reduce the risk of infection in infants born to mothers with hepatitis B by nearly 70%.
Since the universal vaccination of infants against hepatitis B was first recommended in 1991, it has significantly reduced annual cases among children from approximately 18,000 to about 20. However, some, including HHS Secretary Robert F. Kennedy Jr., have raised concerns regarding the vaccine’s necessity and safety despite extensive supporting evidence.
Maternal screening for hepatitis B typically occurs during the early stages of pregnancy, but it can miss infections contracted after testing. Experts underline that vaccinating every baby creates a critical safety net, especially when maternal screenings fail to detect current infections. “We have a duty to protect these little babies,” Fryhofer emphasized, highlighting the need for vigilant post-natal care.
Is the hepatitis B vaccine safe?
The Vaccine Integrity Project found that vaccinating infants against hepatitis B at birth is “consistently demonstrated to be safe.” Reported reactions to the vaccine have generally been mild to moderate, such as soreness at the injection site and low-grade fever, with no significant incidence of severe adverse events. Dr. Anthony Fiore, a former CDC official, endorsed the vaccine’s safety, stating that no long-term negative consequences have emerged, particularly in comparison to those associated with chronic hepatitis B infection.
This ongoing discourse around hepatitis B vaccination reflects broader public health challenges, emphasizing the importance of evidence-based policies in safeguarding health.