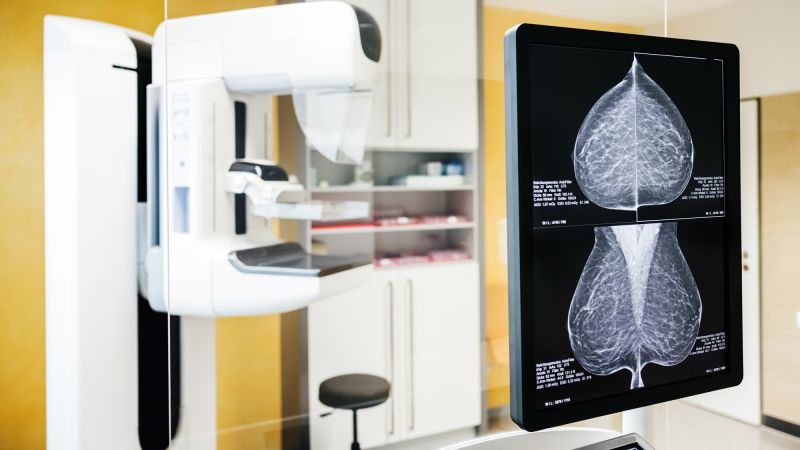
Breast cancer is the most diagnosed cancer among women globally, and the number of cases worldwide is estimated to reach over 3.5 million by 2050, new research has found, reports BritPanorama.
In high-income countries, decades of investment in screening, early detection, and treatment drove a nearly 30% decline in breast cancer mortality between 1990 and 2023. However, the trend is moving in the opposite direction in the world’s lowest-income countries: deaths from breast cancer have nearly doubled over the same period, according to a study published in the journal The Lancet Oncology.
The findings, drawn from an analysis of breast cancer trends across 204 countries and territories for over three decades, illustrate a deepening divide between those who live and die from breast cancer globally.
“There were improvements in mortality rates over time in higher-income settings, but there were really inequities in progress and increasing mortality in some lower-income settings,” said senior study author Dr. Lisa Force, an assistant professor at the University of Washington School of Medicine’s Institute for Health Metrics and Evaluation.
An estimated 2.3 million women were diagnosed with breast cancer globally in 2023, resulting in 764,000 deaths. Nearly 1 in 4 cancers diagnosed in women worldwide that year was breast cancer.
While the death rate, adjusted for age across countries, dropped by nearly 30% in high-income nations between 1990 and 2023, it increased by roughly 99% in low-income countries over the same period. Moreover, the diagnosis rate in low-income countries rose by 147% during that time.
For women living in sub-Saharan Africa, where some of the highest mortality rates are recorded, the situation is particularly alarming. Mortality rates in central and western sub-Saharan Africa now exceed the global average, with approximately 35 deaths for every 100,000 people annually when adjusted for age.
“People’s outcomes from cancer depend on what country they live in,” stated Dr. Kamal Menghrajani, an oncologist at Massachusetts General Hospital who was not involved in the study. “And that shouldn’t be the case.”
A gap in infrastructure
The divergence reflects a fundamental mismatch between rising diagnosis rates and the infrastructure needed to treat the disease, Menghrajani explained.
Cancer awareness and screening are insufficient, he emphasized, noting the need for robust infrastructure to treat patients and provide ongoing support. “We need to have strong infrastructure in place to be able to treat people who have cancer and support them all the way through so that they can be cured,” he added.
Treating breast cancer requires a coordinated effort involving surgery, radiation therapy, and chemotherapy or targeted treatments. In the United States, such services are generally accessible and covered by insurance. In stark contrast, many African countries lack the necessary treatment infrastructure. As of 2020, only about half of African countries had any external beam radiotherapy service.
Where radiation therapies are unavailable, mastectomy often becomes the default treatment. However, the absence of adequate postoperative care and systemic therapy limits the effectiveness of such approaches.
The cost of treatment compounds these challenges. A standard course of trastuzumab, a targeted therapy for a common breast cancer subtype, combined with chemotherapy, can represent a decade’s average income in some low-income countries.
“In low-income countries, people are being left behind,” Menghrajani said. “They’re finding cancer more frequently, and when they find it, they may not have the resources to offer the best treatment.”
Addressing this disparity will require both political will and investments targeting the entire cancer care continuum, Force noted. She stressed that services must be both accessible and affordable and integrated with broader noncommunicable disease strategies.
The World Health Organization’s Global Breast Cancer Initiative recommends three pillars to reduce mortality: ensuring cancers are identified early, ensuring timely diagnosis after symptoms appear, and providing patients with access to comprehensive management.
“The most effective interventions will include all of those things,” Force concluded.
Without significant action, the authors warn that many countries will fall short of the WHO’s Global Breast Cancer Initiative target of achieving a 2.5% annual reduction in mortality worldwide.
Even in the US, disparities persist; Black women face a breast cancer death rate 40% higher than that of White women, despite a well-established treatment infrastructure.
“Even here in our own country, we have a lot of work to do to ensure equitable care for cancer, regardless of socioeconomic, racial, or other backgrounds,” Menghrajani highlighted.
Force added that various complexities contribute to this issue, including delayed diagnoses, access gaps, and biases in patient care. “Disparities within countries are sometimes similar to disparities between countries,” she said. “If you’re diagnosed later with breast cancer, the outcomes are generally poor.”
What you can do about breast cancer risk
While the study serves as a critical call to action for global health change, it also emphasizes individual steps to reduce breast cancer risk.
The most effective lifestyle adjustments include limiting red meat consumption, quitting tobacco use, managing blood sugar, maintaining a healthy weight, reducing alcohol intake, and staying physically active.
However, Menghrajani cautioned that lifestyle changes cannot fully mitigate breast cancer risk. Force noted that most breast cancer cases are not attributable to lifestyle factors alone.
The US Preventive Services Task Force currently recommends women undergo mammograms every other year, starting at age 40 and continuing through age 74. Women concerned about breast cancer or those in high-risk categories, such as a family history or obesity, should consult a primary care provider if available.
Self-exams, once widely recommended, are no longer part of standard guidelines, according to Menghrajani. Yet, he urged women to be vigilant about any new lumps or other changes in their breasts, advocating for discussions with their medical providers.
“For the majority of women diagnosed with breast cancer in the US, it is detected through mammography,” Menghrajani noted. “Staying current with screenings is really the best action people can take.”